6.075 views (website & LinkedIn) – 14/1: toevoeging bewijslast/bronmateriaal en datering, lezersstatistiek; verzoek om donaties van dit onafhankelijk onderzoek naar het presteren van de Nederlandse gezondheidszorg – Top20 (16)
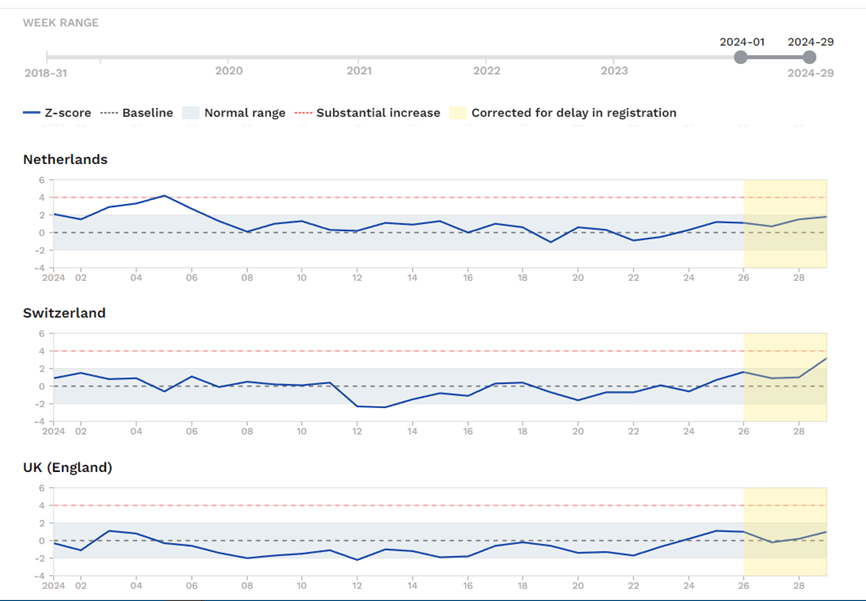
Al jarenlang bericht onderzoeker Gijs van Loef over de Excess Mortality Ranking (‘oversterfte’) in Nederland. Hij concludeert steeds weer dat op basis van Eurostat-gegevens Nederland sinds corona een koppositie inneemt bij oversterfte in vergelijk met overige Europese landen. Het RIVM/CBS (of anderen) zijn aan zet om deze sterftecijfers te analyseren, want de vraag blijft liggen: hoe komt dít? Wanneer een individuele Nederlander in nood lijkt, volgt al snel een alert, politiebericht of zoektocht. En bij een méér dan gemiddelde oversterfte? - Anton Maes, zorgenstelsel.nl
Dank je, Gijs en ja: ik bedoelde West Europa - Jos de Blok
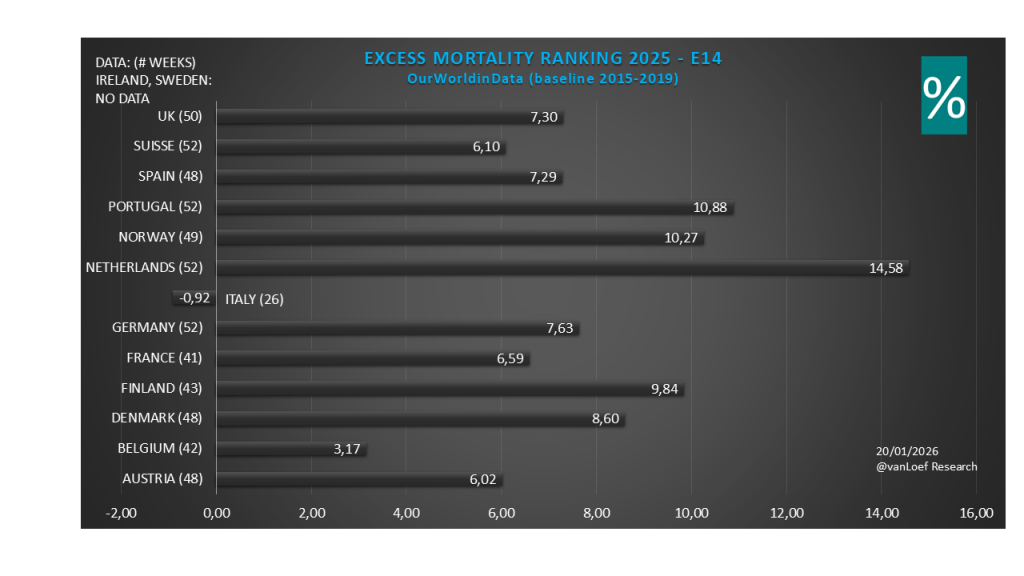
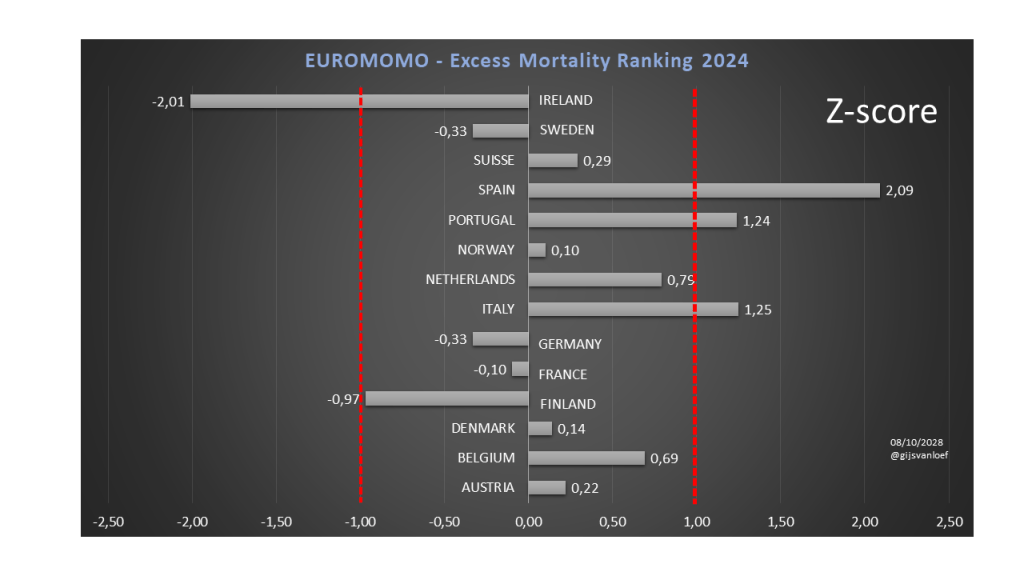
Zojuist beluister ik – met stijgende verbazing – de podcast van NPO Radio1 van 14 feb. ’25, FEIT of FICTIE. Jos de Blok wordt geciteerd: “Nederland had tijdens de coronaperiode de grootste oversterfte van Europa!”. Men is dit gaan uitzoeken. De bijdrage van Prof. Anton Kunst (sociaal epidemioloog) is glashelder, daar valt niets op af te dingen. Maar Ruben van Gaalen slaat de plank ook hier weer mis. Hij zegt: “Nederland was qua oversterfte een middenmotor in Europa.” Let wel. Het is weinig zinvol om het over geheel Europa te hebben, want de verschillen in kwaliteit van zorgstelsels is enorm. Iedere zorgeconoom (en beoefenaar van aanverwante kennisgebieden) weet dat het alleen zinvol is om moderne, West-Europese landen onderling te vergelijken. Van Gaalen noemt landen als Roemenië en Bulgarije. Maar v.w.b. West-Europa beweert hij dat Portugal, Spanje, Italië en Engeland een hogere oversterfte hadden. Dit is pertinent onjuist, uitgaande van het geëxpliciteerde tijdvak 2020 t/m 2023.
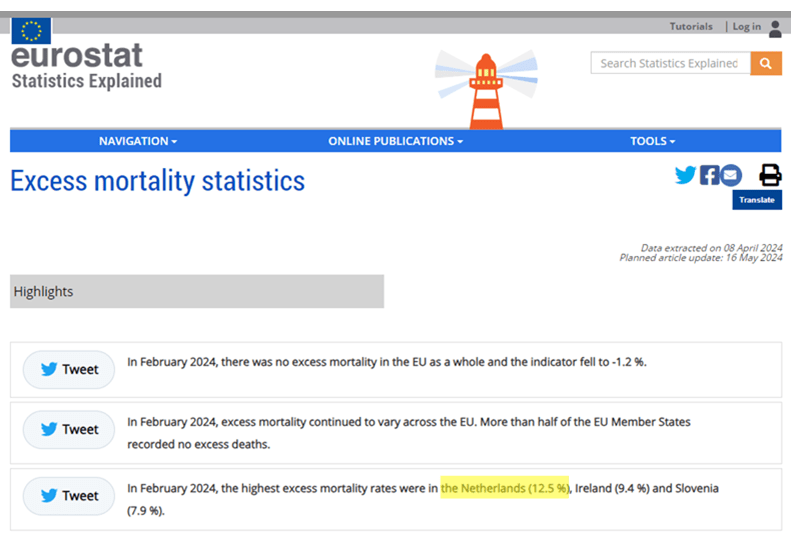
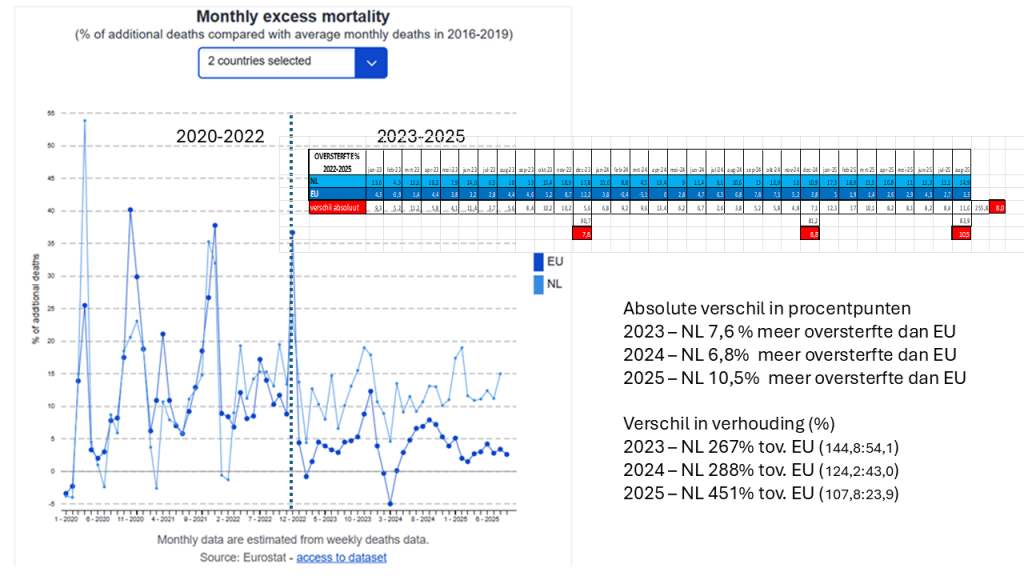
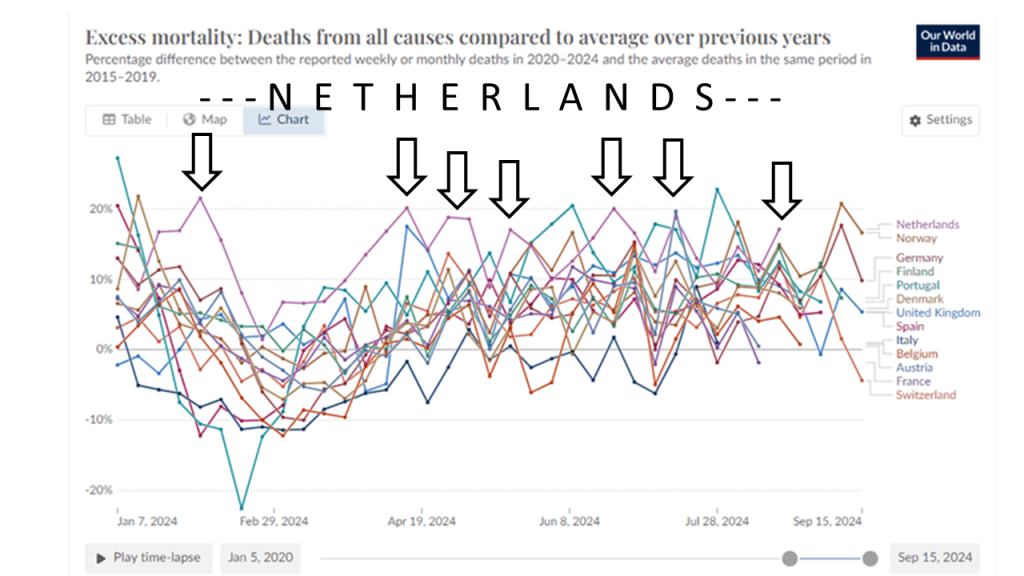
Nederland heeft op elk moment in de tijd, gemeten vanaf de periode 2020-2023 de grootste oversterfte zo is gebleken o.b.v. de openbare internationale statistieken en dit is zelfs tot op heden het geval! vanLoef Research heeft dit systematisch blootgelegd en nieuwe data hebben dit steeds weer bevestigd.
Jos de Blok had strikt genomen geen gelijk, maar misschien bedoelde hij eigenlijk West-Europa? Maar Ruben van Gaalen had zeker ongelijk.
Bijgaand de volgende, eerder gepubliceerde statistieken.
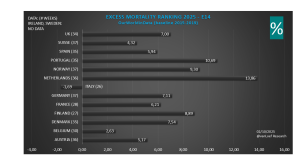
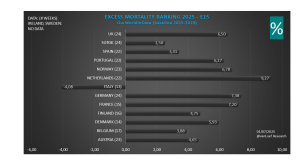
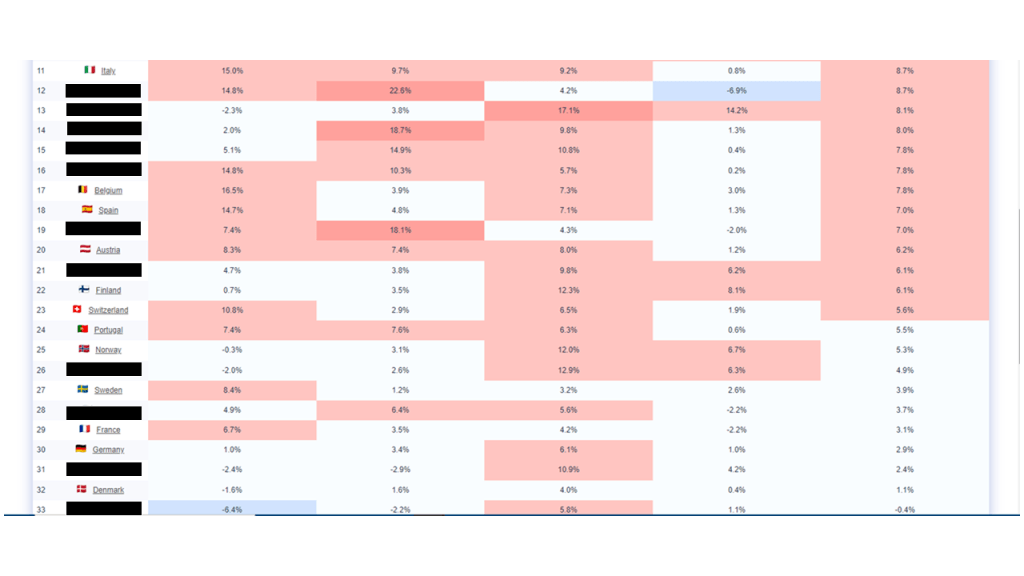
Excess mortality 2020 t/m 2023 Eurostat (baseline 2016-2019)
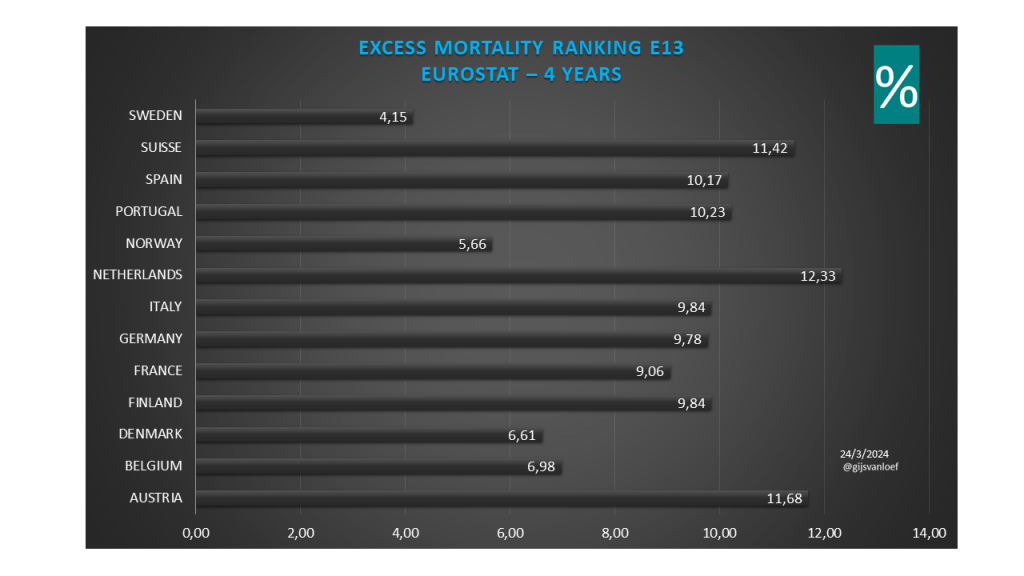
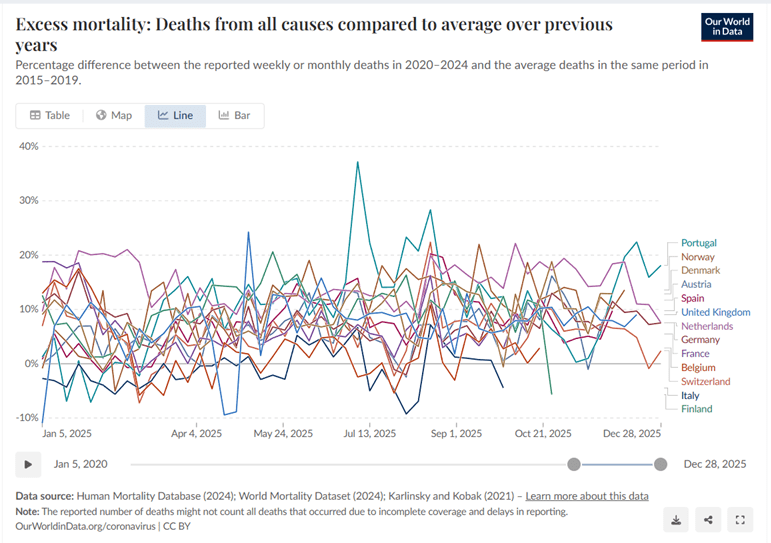
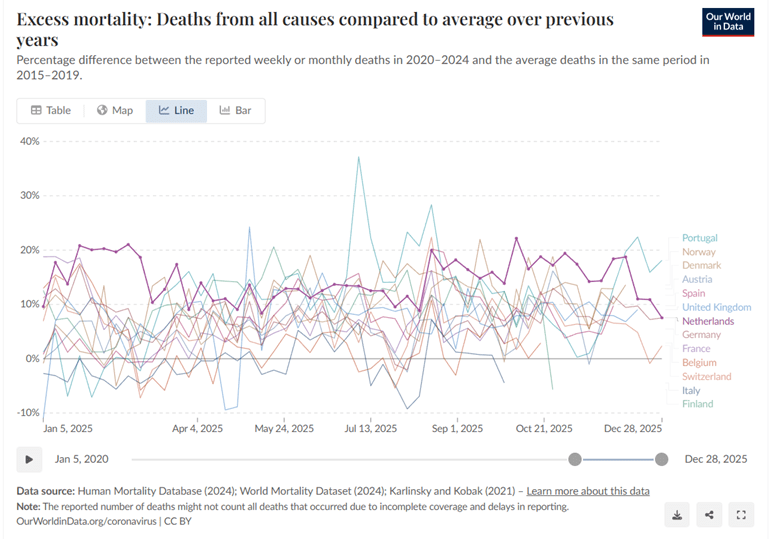
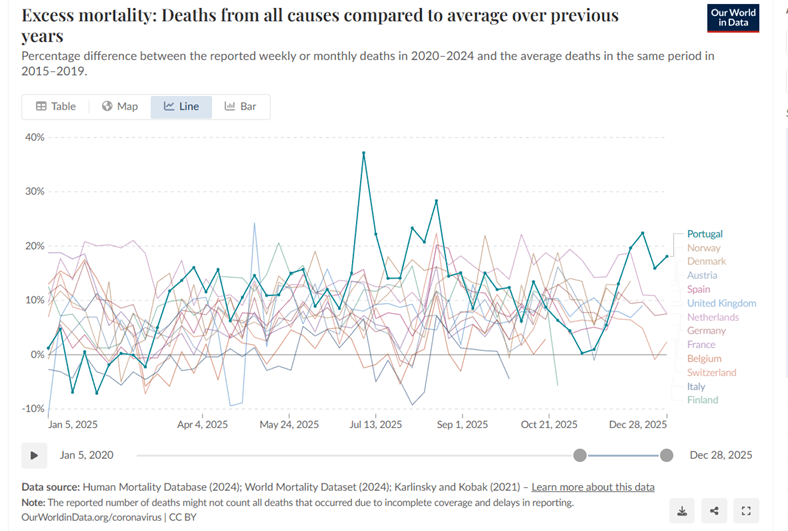
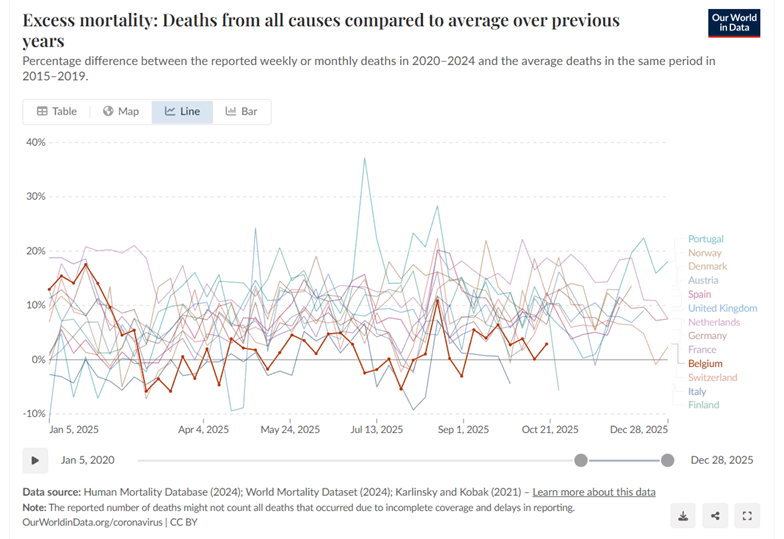
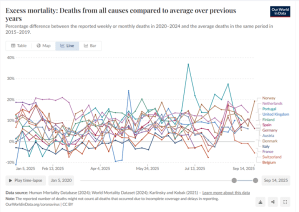
Excess mortality 2020 t/m 2023 OurWorldinData (baseline 2015-2019)
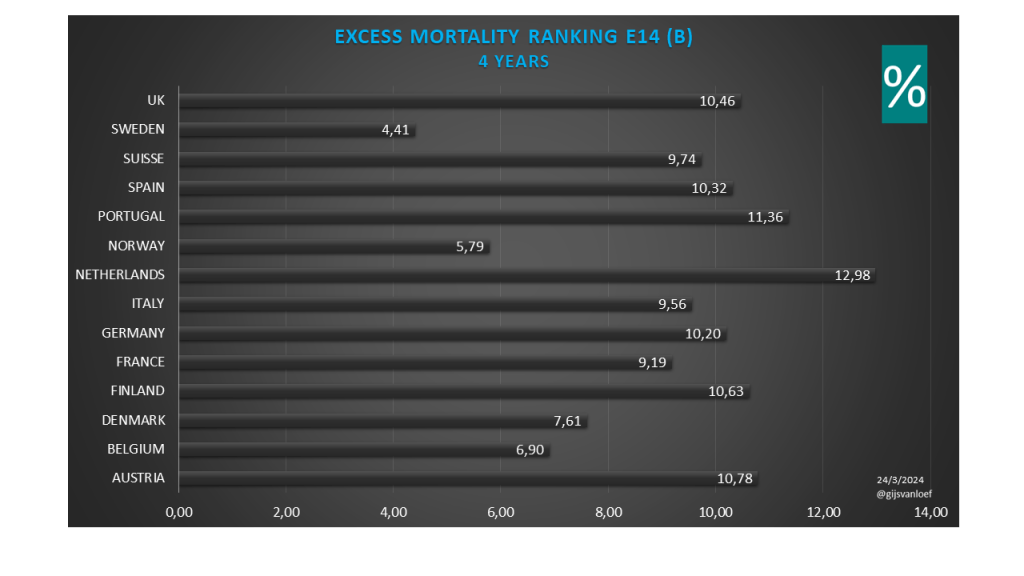
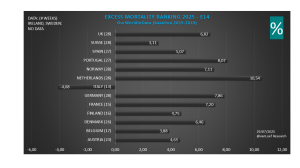
Excess mortality 2021 t/m 2023 Eurostat (baseline 2016-2019) – 3 vaccinatiejaren
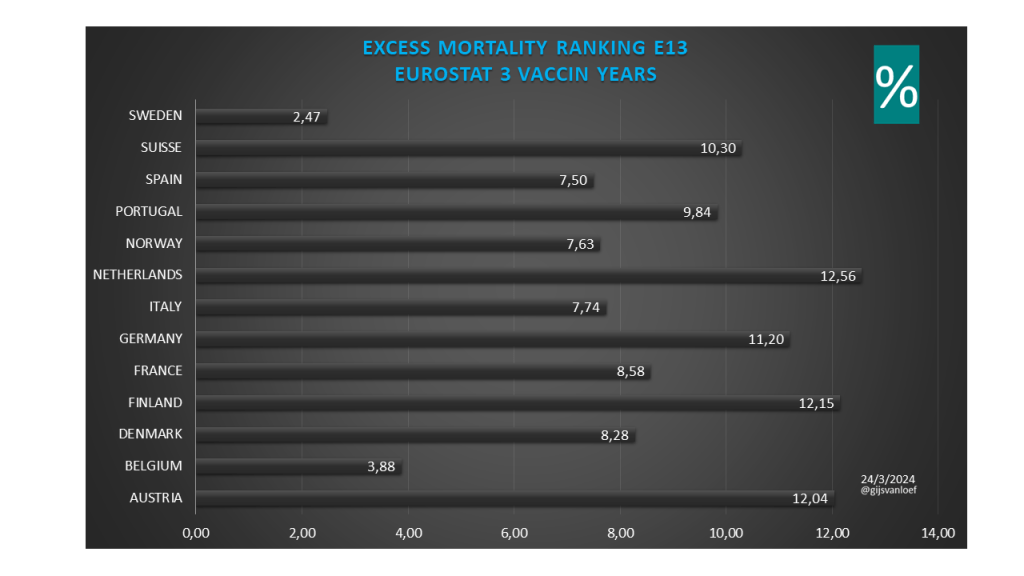
Excess mortality 2021 t/m 2023 OurWorldInData (baseline 2015-2019) – 3 vaccinatiejaren

Excess mortality 2020 t/m 2024 Eurostat (baseline 2016-2019)
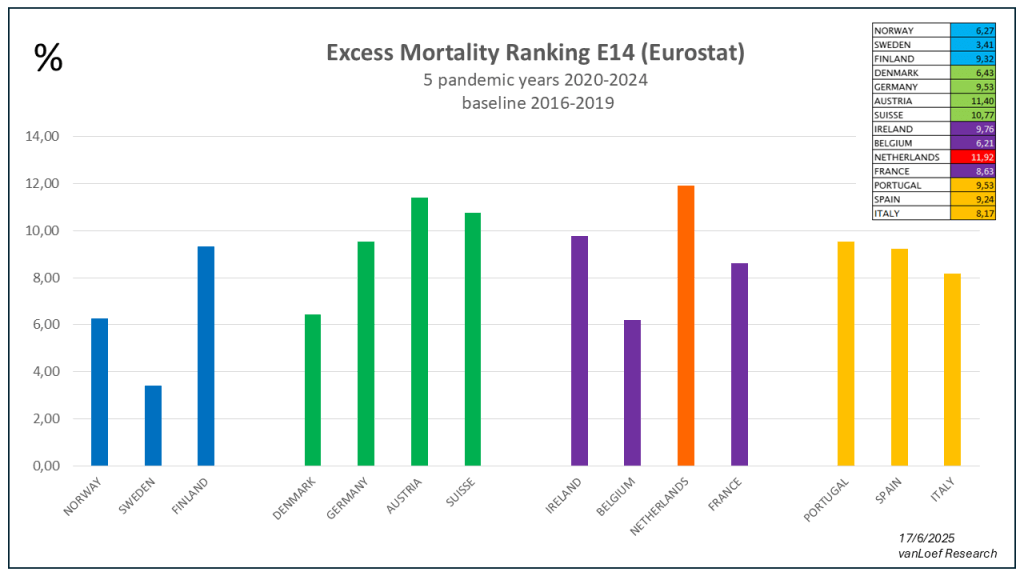
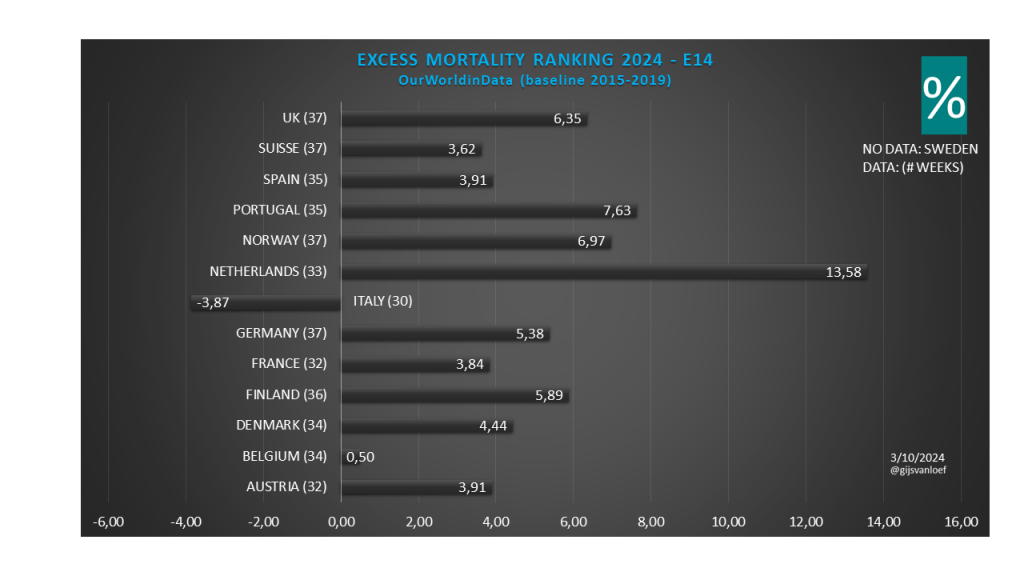
Excess mortality 2020 t/m 2024 OurWorldinData (baseline 2015-2019)
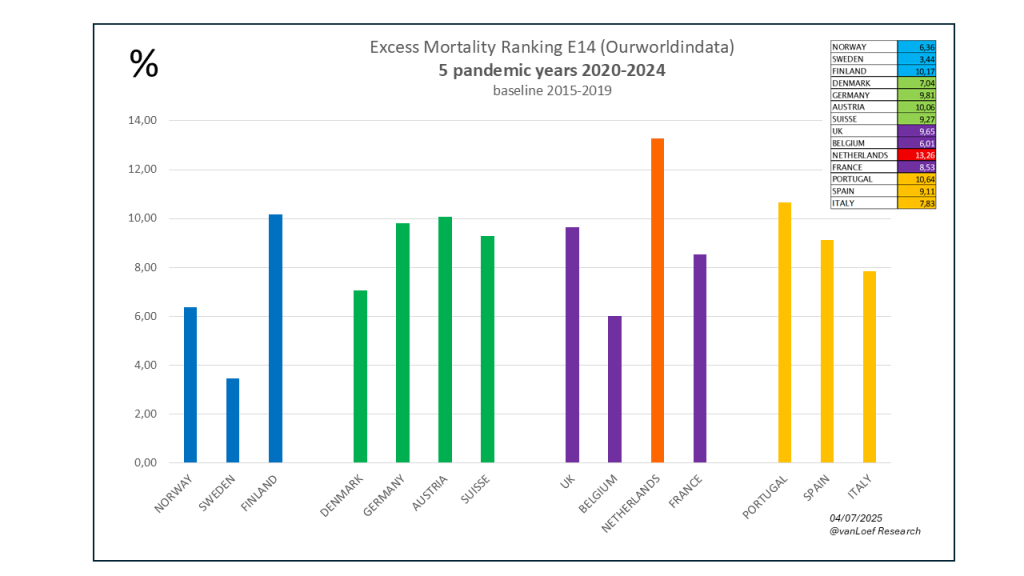
Toelichting. Alleen bij de vierde statistiek scoort Finland nipt 0,01% hoger dan Nederland.
Wat doe ik? Beoefening van kritische wetenschap. Mijn bijdragen liggen in de onafhankelijke analyse van de werking van de marktgedreven zorg op basis van een integrale kennisbenadering en analyse van cijfers/kengetallen en oplossingen - de ontwikkelde kengetallen (oa. oversterfte>dalende levensverwachting; arbeidstekort) worden inmiddels breed geaccepteerd. Tevens houd ik mij bezig met het ontwerp van een beter zorgstelsel (publiek primaat; kwalitatief, financieel).
Wat kunt u doen? Steun dit onafhankelijk onderzoek door het te delen en/of neem contact met mij op.
U kunt ook doneren en dan een bijdrage storten op bankrekening NL93 INGB 0104514876 t.n.v. van Loef Research & Consult.
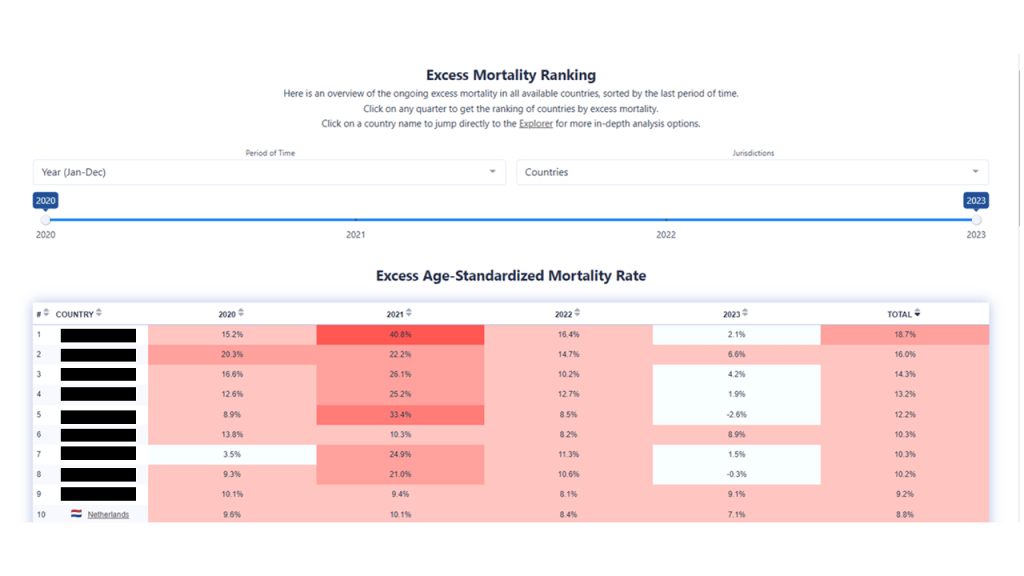
Door 3 cruciale kengetallen te onderbelichten (extreem ziekteverzuim zorgsector indiceert dat de sector ziek is; oversterfte en achterblijvende levensverwachting (causaal verband) indiceren dat de 'opbrengsten' van de zorg onvoldoende zijn) werkt CBS mee aan het verbloemen van het falen van het zorgsysteem. Berichten van een bijzonder hoogleraar in dienst van het CBS over de levensverwachting bleken misleidend.
Het zijn de harde conclusies van vanLoef Research op basis van zelfstandig onderzoek naar de berichtgeving van het CBS in de afgelopen vier jaar.
uit: https://gijsvanloef.nl/2025/03/19/cbs-persisteert-in-dubieuze-berichtgeving-sterfte/
Bronnen (oudste eerst)
maart 2024
sept. 2024
dec. 2024

mei 2025
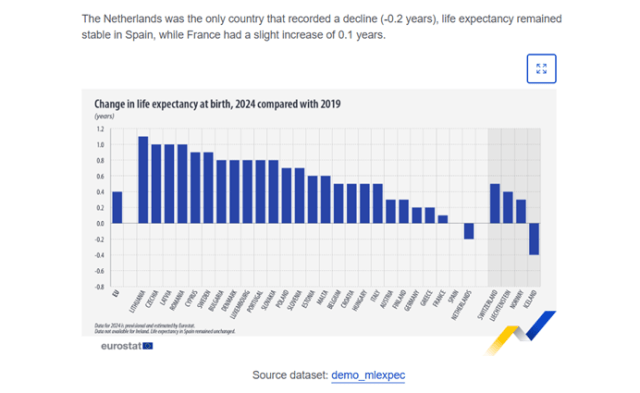
sept. 2025: Eurostat meldt gedaalde levensverwachting Nederland

december 2025
Podcast NPO Radio1